All about IUGR pregnancy, delivery, and postpartum life. Find out what to expect in each stage of Intrauterin Growth Restriction.

Post Contents
BIO
Hi! My name is Chantal, a 29-year-old mom to my 19 month old pandemic baby. My husband and I, along with our baby girl and puppy, Milo, are based in Ontario, Canada. My baby was born in October 2020 during the height of the Second Wave of the COVID-19 Pandemic. I was so excited when Valerie approached my Babywise group inviting us to share some of our unique parenting experiences! Read along to find out how we navigated finding out that our baby was IUGR during this challenging world event.
Please note that I am in no way a medical expert and this blog is an account of my personal experience. I am sharing the choices we made with the tools and knowledge we had access to. Always consult with your own healthcare professional.
Intro
We found out our baby was IUGR when I was 32 weeks pregnant, placing me in the high risk category. I was left with so many questions about what that would mean and what would come next. The answers that the doctors provided were vague and left me feeling unprepared. So, within this blog, I will chronicle my journey in hopes of giving you a little clarity on what might be expected for your IUGR Baby.
What is IUGR?
IUGR stands for intrauterine growth defect/or intrauterine growth deficiency. This means that our little one was growing slowly and didn’t weigh as much as the doctor expected for each stage of pregnancy. When we got this news we were nervous; we didn’t know what would come next!
I remember people telling me that my stomach looked smaller than other pregnant women in the middle of my pregnancy. While I’m sure it was well-meaning, these comments left me with an overwhelming sense of guilt. “Am I doing something wrong?” I started “carbing” up and drinking meal supplements to help with my own weight gain. But the reality is that this was a medical condition that was totally out of my control.
Pregnancy
Once we were given this diagnosis, our pregnancy journey started to look very different. The doctors gave me a couple of options. Their first option was to deliver my baby early at 34 weeks. Although my doctor really encouraged this option, it just didn’t sit right in my heart. At the time of diagnosis, I was only 32 weeks along and I felt so unprepared to have our baby…I thought I still had nearly two months of pregnancy left! This was a path I wasn’t enthusiastic to take unless I really had to.
Alternatively, the doctors informed me that I could monitor our baby’s growth for as long as possible and that they would continually assess when it was time! I chose this path, not knowing what it would entail emotionally.
I was asked to visit the High Risk Clinic at my local hospital every other day, we would monitor during each visit and reassess how much longer our baby could stay inside my womb. My pregnancy was during the height of COVID and my husband was not allowed to join me during any of my visits. We were monitoring for a trajectory of weight gain and they informed me that when they observed a plateau, we would have to schedule a date to induce.
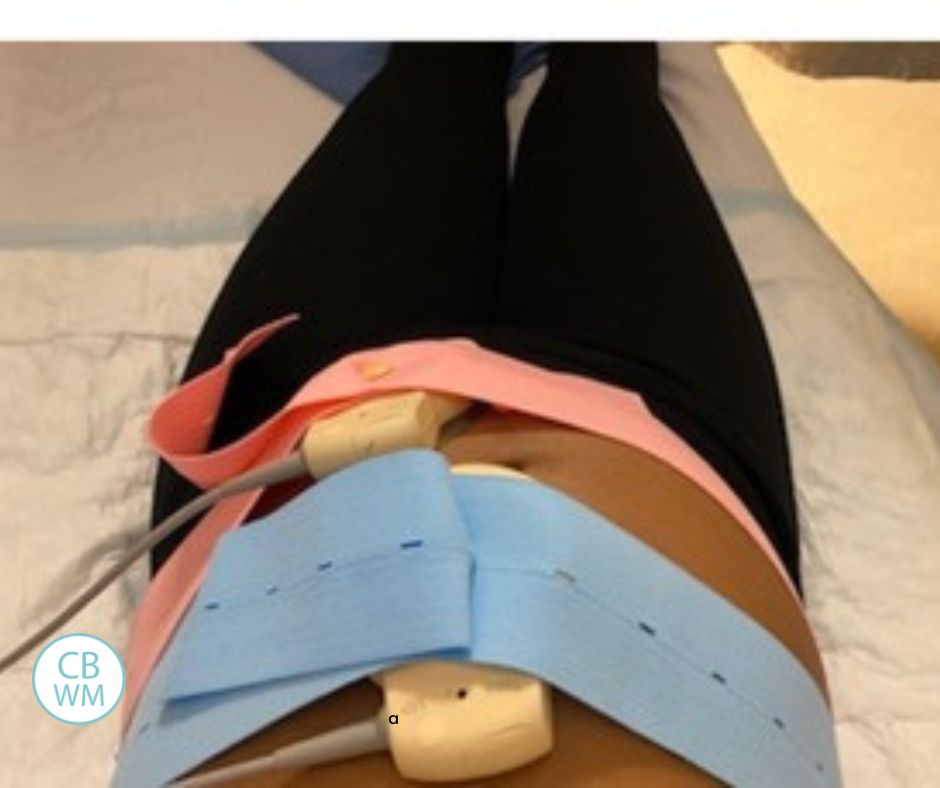
Each week, a nurse would conduct an ultrasound to determine how long our baby was and how much she weighed. For reference, at 33 weeks my baby was less than 3 pounds. I would also go in for a NST or Non-Stress Test, where they would monitor our baby’s heartbeat and movement by placing two bands across my belly and a fetal heart rate monitor within them. I was connected to a TV-like screen that tracks the baby.
At 36 weeks, my OB said she’s noticed some stagnancy in growth and it was time to schedule a day for delivery. She was very nonchalant about it, asking if I was free on Friday like she was scheduling a dinner date. I answered saying I was, thinking she was just going to schedule another appointment that had become very routine to me at this point. When she started looking at times for delivery, I became so overwhelmed…this was actually happening! I begged for one more week, with the hopes that our baby’s lungs and all other organs would have enough time to finish developing and the doctor allowed me this grace with the understanding that I should have a hospital bag ready in my car at every visit.
Birth
At 37-5 it was time! My husband and I were so excited the night before that I couldn’t sleep (although thinking back to all the interrupted sleeps to come, I should have tried harder!). We googled all the hospital bag blogs, packed all the things, got the nursery ready, cleaned the house, put a few dinners in the fridge, and I was ready to go!
We left the house to go to our local hospital. My appointment was at 10 am, now to remind you, this was in the height of COVID. My husband was asked to stay in the waiting room while they performed the induction. The doctor manually opened up my cervix (boy, was that uncomfortable) and just like that, we were two-centimeters along. I should mention, that between 36 and 37 weeks, I drank Raspberry tea everyday, to help our baby drop. My goal was to have a vaginal birth, so I googled all of the things to support a “pre-term” birth. This was helpful because we didn’t need to use the Balloon Method of induction.
Once I was officially admitted, my husband was invited to join me in the Labour and Delivery room. We were all hooked up and ready to go! Things were moving slowly at first and my contractions (while painful as all hell) were far apart. I wasn’t dilating as quickly as they wanted. This was concerning because I really waited until the last possible moment to have our baby, so the doctors were wanting things to move along swiftly. At 3:30 pm the doctors manually broke my water. At 12:30 am it was time to push! My sweet angel was born at 1:43 am.
Once she came it was an emotional whirl wind! I was crying, the nurses latched her on to me for the first time and, in that moment, I became MOM. The best title that I never knew I needed.
My sweet girl was born at 4 pounds and 10 ounces.
We spent an hour with her before she was taken to the NICU.
NICU
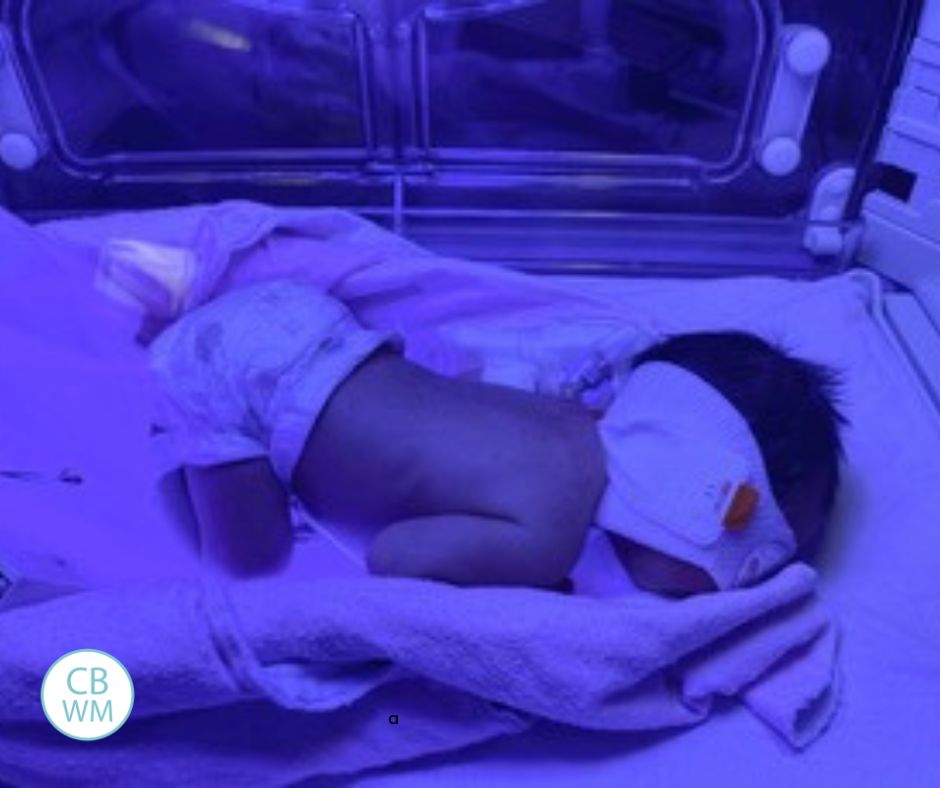
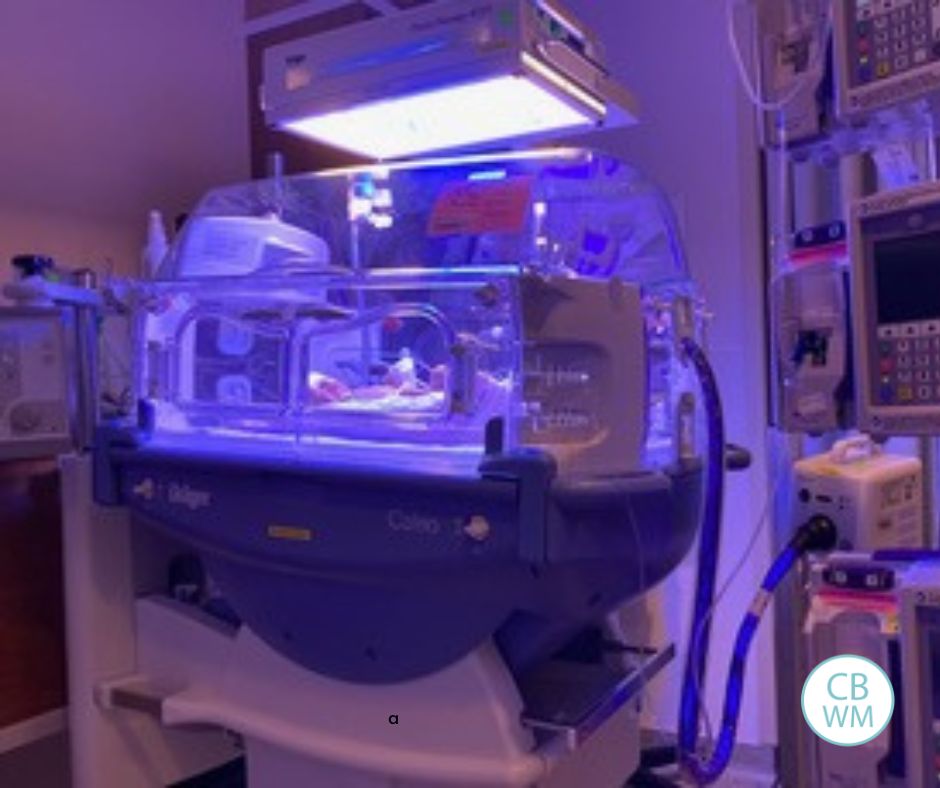
Our tiny girl was just that, so tiny. She was taken to the NICU where she spent one week. She had jaundice and low sugars. The nurses and doctors were also monitoring her weight gain and food intake.
That first night, my husband and I were in the postpartum delivery room while our baby was on the other side of the hospital floor in the NICU. That first hour was the only time we were allowed to be together as a family until she came home (re: COVID protocols). We were only allowed in the NICU one at a time and could only take her out of the incubator when it was time to feed. We stared at our sweet angel on the other side of the blue screen, as the UV rays helped make her strong and the IV helped nourish her. This was particularly challenging, as you could imagine. Not being able to hold our baby for as long as we wanted and being separated from each other was heart-wrenching.
Once we were discharged from the postpartum room, my husband and I were only allowed back in the hospital one at a time. My husband would drop me off at 7am for the first feed of the day and I would sit by my baby’s side until he came home from work and we switched. It was the longest week of our lives; we felt so disjointed because we didn’t have time to bond as a family. What we didn’t know until we got home is how much knowledge we gained from spending time alongside the nurses. From swaddling and diaper changes to the basics of breastfeeding. I wouldn’t say it was a blessing in disguise but I would say we were blessed with the opportunity to learn.
Lactation and Weight Gain
Once we got home the second leg of our journey began! We started with our routine check-up with my family doctor within 72 hours of coming home. At that visit, I was referred to the Lactation Consultant to monitor our baby’s intake and weight gain.
We were on a tight feeding schedule. Our schedule was a 2.5 hour rotation: feeding for 40 minutes, 20 on each side with a “top up” (described in further detail below), followed by pumping to keep my supply high. We were given sheets of paper to take note of each time we fed our baby and for how long. (We quickly switched from sheets of paper to downloading the Huckleberry app. This app allowed us to time breastfeeding, alert us when it was time to feed and gain, timing naps, and so much more. There are so many things to keep top of mind when you are a new mom, Huckleberry helped me stay on top of it all.)
My daughter was small, and she was staying small. When our baby wasn’t gaining enough weight, as quickly as the doctors wanted, we started using my milk supply to top up with a supplemental nursing system (SNS). This was a tube, connected to a syringe that I would place over my nipple into our baby’s mouth to increase the amount of milk she was getting per feed. This is a great trick to help with breastfeeding. Once that milk started flowing into our baby’s mouth from the tube, she latched and started drinking away.
The lactation consultant followed us for the first three months. When my daughter was born, she wasn’t even near the low end of the weight/growth chart. There were times in my journey we saw her weight plateau and decreased before eventually charting in a desirable direction.
I can’t begin to describe how emotionally tumultuous this time of my life was; becoming a new mom, overwhelmed with obsessively monitoring my milk supply and my baby’s intake, isolated due to COVID, plus all the other things that come with transitioning to motherhood.
We don’t all have a village but seeking out other mama’s you can connect with was transformative for me. I strengthened relationships with all the new parents I knew and built a community by connecting with people online and in my neighbourhood. People that I never spoke with before became trusted confidants over time!
It was important for me to learn from other moms that our relationships pivot and evolve post-motherhood, that we are all working harder than we ever thought we would be, and learning the tips and tricks that make it more manageable. I know it can be intimidating to approach someone but other new moms are also looking to connect. And we all have the journey of motherhood in common!

Babywise and IUGR
When I discovered Babywise, I was so overwhelmed by all the new responsibilities and the chaos of each day. I was drowning in different messages from my family doctors that suggested I give up on my breastfeeding journey to my LC’s opinion that it was too early to encourage longer stretches of sleep during the night, to feelings of isolation during new motherhood.
Babywise helped me organize these chaotic days, got me on a schedule I could actually follow, and showed me there could be some calm within the chaos.
Such a simple thing, such as a directed wake up time each day, made my days become so much more uniform. Our naps all became more consistent, routines started to emerge and I started to feel in control again, for the first time since I was 32 weeks pregnant. It was transformative!
Conclusion
Getting the diagnosis of IUGR can be daunting, I know. There is simultaneously a lack of information and an overload of misinformation out there. I hope my blog was able to provide some insight on what an IUGR can look like; from routine ultrasounds and NSTs, to induction, to gaining weight after birth. There is a lot that will be asked of you as an IUGR mama. But you have the strength to prevail. By seeking out information, you are already making sure you are well-prepared for your baby! If you ever wish to connect further, send me a DM @chantalmarie___ and I would be happy to share with you. You’ve got this, mama!
Related Posts

